The problem of joint diseases is always relevant. After forty years, about a third of all people begin to feel pain when moving, and after fifty, more than half of the population begins to feel pain. Doctors call osteoarthritis the gradual destruction of cartilage, ligaments, bones and soft tissues around the joints.
How can you prevent this condition? And what treatments will help relieve pain when the disease has already developed? To answer these questions, it is first necessary to understand the difference between arthritis and osteoarthritis, the most common joint pathologies.
What is arthritis?
The main difference between arthritis and osteoarthritis can be seen in the names: acute and sudden diseases end in "-itis"; with "-de" – slow-moving diseases, chronic processes.
Arthritis is an inflammatory lesion of the joints that occurs due to a malfunction of the immune system due to infection (for example, sore throat or otitis media), trauma, metabolic disorders, hypothermia, stress or other reasons (including autoimmune ).
The first signs appear like this:
- sharp pain in one or more joints (often not only during movement), especially early in the morning;
- enlargement, swelling, edema, redness of the sore joint;
- a noticeable increase in temperature at the site of inflammation.
The inflammatory processes caused by arthritis can affect the entire body. In this case, the patient feels a high fever, chills, loses strength and may experience inflammation of other organs (eyes, genitourinary system, including heart, lungs, liver and kidneys).
Arthritis has several dozen forms. The most common are:
- rheumatism– inflammation of the connective tissue of large and medium joints that occurs after infections;
- rheumatoid arthritis– a slow autoimmune process that symmetrically affects several joints at the same time; causes the appearance of "nodules", pain, loss of mobility; can cause inflammation of many organs;
- drop– caused by the accumulation of uric acid in the blood and salts in the joints; most often it begins with sharp pain in the big toe joint;
- reactive arthritis– occurs against the background of damage to the body from infections (chlamydia, streptococcus, etc. );
- infectious arthritis– begins due to a bacterial infection of the joint itself.
What is osteoarthritis?
Unlike arthritis, osteoarthritis is not accompanied by inflammatory processes. It causes poor circulation in the joint, which causes the cartilaginous parts to begin to dry out.
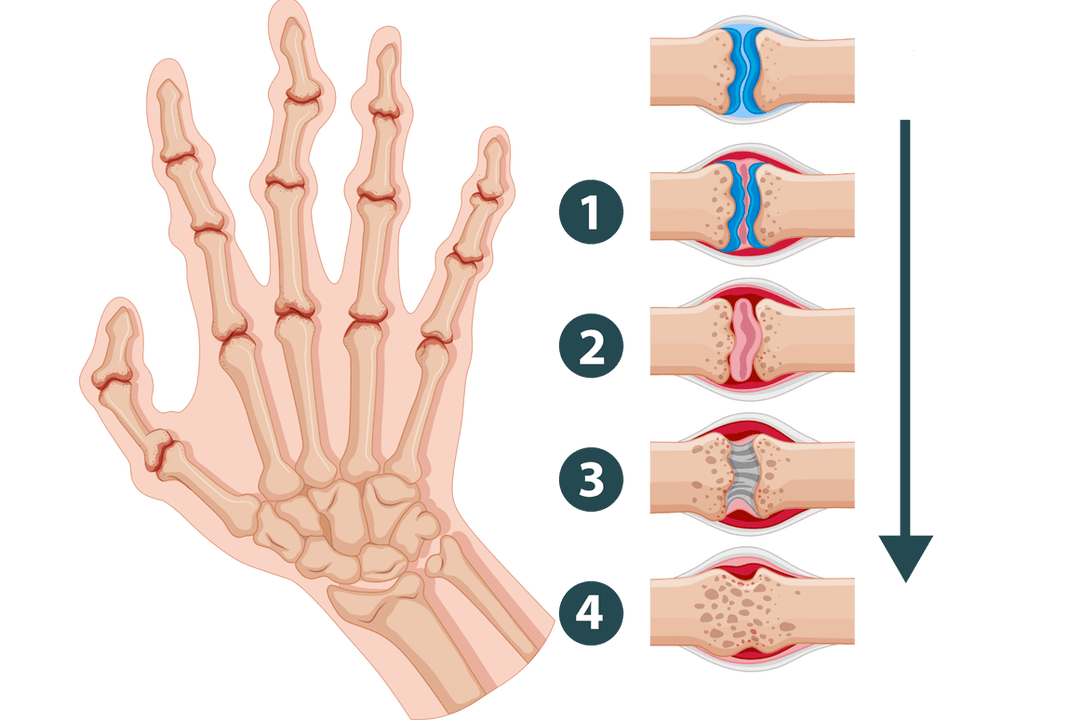
Osteoarthritis is a disease that deforms and destroys joint tissue. With it, the connecting layers dehydrate, become thinner and "wear out". The bones begin to touch each other, causing pain and making it difficult for the person to move.
Signs of joint osteoarthritis are:
- After a long period of immobility (for example, a night's rest), the joint "freezes", but then develops rapidly when activity is resumed;
- the functioning of the joint is accompanied by strange sounds (clicks, creaks, squeaks);
- physical activity causes pain.
What are the differences between arthritis and osteoarthritis?
Both diseases affect the joints. But they are caused by different reasons, proceed differently, and can have very different consequences. Only a correct diagnosis, based on the difference between arthritis and osteoarthritis, can prevent irreparable damage to the body.
It takes time for cartilage tissue degeneration to develop sufficiently and bone deformation to begin. Therefore, chronic osteoarthritis usually manifests itself in old age (after 60 years, less often after 50). The most susceptible to changes are the joints that constantly work under load: the fingers of musicians, the knees of athletes and loaders, the ankles of people who walk a lot or work standing, etc.
On the contrary, arthritis can occur even in a child. The inflammatory process causes pathology of the synovial membrane, saturated with blood vessels and joint fluid (while in osteoarthritis it is simply produced in insufficient quantities). Unfortunately, almost one in five cases of disability in the world is caused by various forms and complications of arthritis.
Inflammation can affect not only the joints, but also other tissues with active blood circulation: blood vessels and heart, lungs, abdominal organs, eyes, urinary system, etc. On the other hand, osteoarthritis is limited by local mechanical damage to bones and the formation of osteophytes in areas of deformation of the joints. Although in late stages and advanced forms, the disease can also cause disability, completely immobilizing the person's limbs.
How do arthritis and osteoarthritis manifest?

Let's compare the external manifestations to clearly explain the difference between the symptoms of arthritis and osteoarthritis.
- Pain. In the initial stages of osteoarthritis (which lasts for years), joint pain appears during physical activity and disappears with rest. It is rarely sharp and strong. Even as the disease progresses, when pain can appear even with small movements and even at rest, it is usually enough to give the body a comfortable position for the pain to disappear. With arthritis, the patient is bothered by attacks of acute pain of great force, which can only be extinguished with special medications. A characteristic symptom is pain during rest, especially early in the morning.
- Clicking, squeaking, creaking of joints.. In joints affected by osteoarthritis, the cartilage layers are destroyed. They stop protecting the heads of the bones from contact with each other. Therefore, when moving, the bones touch and rub, producing harsh, dry sounds. The more the disease progresses, the louder and louder the joints click. Arthritis is not usually accompanied by these symptoms.
- Deformation of the joint and surrounding tissues.. The development of osteoarthritis over time causes a change in the shape of the bones: their heads begin to crumble and wear out, and osteophytes may appear. Sometimes in the acute stages there is swelling and pain, but these symptoms are not permanent. But a joint affected by arthritis becomes inflamed and swollen. Swelling and compaction occur. The skin becomes red and hot.
- Limited mobility. Osteoarthritis causes stiffness in a specific joint that goes away with movement. In deeper stages, stiffness increases, flexion amplitude decreases, and ultimately leads to immobility. With arthritis, you may feel stiffness throughout your body, and attempts to move will cause sharp pain.
- Changes in blood composition.. Osteoarthritis is not an inflammatory disease, so it is not reflected in the analysis. Arthritis causes a significant increase in the erythrocyte sedimentation rate, indicating an active infectious and inflammatory process.
Therefore, the symptoms of osteoarthritis in the early stages can rarely cause serious anxiety and discomfort. This leads to a careless attitude and late diagnosis of the disease, which complicates subsequent treatment.
Causes of osteoarthritis
There are several factors that increase the risk of pathological changes in the joints and surrounding tissues: constant overload, imbalance of the immune and hormonal systems, poor physical fitness. Therefore, to prevent diseases, it is necessary to periodically follow these recommendations:
- Maintain moderate physical activity through simple exercises, walking, swimming, etc. This will help you get rid of excess weight, improve blood circulation, strengthen muscles and therefore relieve stress on the joints.
- Try to eat healthy foods. Fatty foods, red meat and alcohol can be harmful. On the contrary, seafood, fruits and vegetables and dishes containing cartilage and gelatin will be beneficial for the body. It is important to drink plenty of clean water (2-3 liters a day).
- Choose suitable clothing and shoes: comfortable heels, warm enough, that do not restrict movement.
- If possible, avoid stress, disturbances and other "shocks" to the body.
However, if a person has already been diagnosed with arthritis or osteoarthritis, before performing such simple actions, he or she should consult a doctor. In some cases, conventional prevention can also cause harm and worsen the condition.
But how are arthritis and osteoarthritis treated? What is the difference? The causes of these pathologies differ: immunological processes, fight against infections in the first case versus cartilage malnutrition in the second. Therefore, the ways of dealing with them will be different. To choose the right course of action, you must first make an accurate diagnosis.
To do this, it is best to undergo an X-ray and MRI in combination with laboratory tests of blood and urine. After studying the results, the doctor will prescribe appropriate recommendations.
Arthritis treatment
If the acute form of the disease is caused by an infection, it can be cured with antibiotics. But in this case, it is important to accurately select the drug: it is necessary to neutralize pathogenic bacteria before the pathology of the joint becomes irreversible. The course is complemented by anti-inflammatory and immune-supporting medications.
In the case of chronic arthritis (for example, rheumatoid), treatment must be carried out regularly throughout life. The most commonly used are corticosteroids, cytostatics and modern biological products. These are quite powerful drugs, so to ensure that they do not cause harm to the body, it is essential to correctly calculate the doses, frequency and duration of their use.
For severe pain, your doctor may also prescribe painkiller treatment. And complementary support methods are necessarily recommended: diet, physiotherapy and a course of physiotherapy. If the inflammation has spread to other organs, the patient should be referred for additional specialized examinations.
Osteoarthritis treatment
Modern methods make it possible to almost completely eliminate the manifestations of the disease if the diagnosis is made at an early stage and the patient's age does not reach forty years. To do this, in addition to standard control of tension in the joint and treatment with medications (which initiate regeneration, restore nutrition and hydration of the cartilage), the patient may be prescribed mud wraps, electrophoresis and acoustic therapy (which affects the affected area). tissue with low frequency sounds).
In older people or in advanced forms, osteoarthritis cannot be completely cured, although it is possible to achieve a significant improvement in the condition and slow down the destructive processes in the joint. This requires strict adherence to the doctor's recommendations: regular use of medications (for example, chondroprotectors), maintaining a healthy lifestyle, timely completion of prescribed procedures and control of joint load.
In osteoarthritis, the main attention is paid to the restoration of the cartilage layer. If there are concomitant symptoms of inflammatory processes, antibiotics or corticosteroids can be prescribed to relieve the acute stage and proceed to the main treatment regimen. In some severe cases, surgery and even the implantation of an artificial joint may be necessary.
























